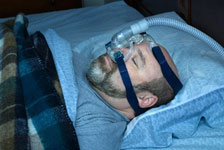
 Snoring and Obstructive Sleep Apnea are separate but sometimes associated disorders that result from upper airway obstruction. Snoring results from multiple factors that may include nasal airway obstruction, obesity, mouth breathing, enlargement of the adenoid, tonsils, and base of the tongue, and vibration of structures such as the uvula and soft palate. Obstructive Sleep Apnea (OSA), or cessation of breathing during sleep, may result from the same factors, but is a more serious health condition. Medical studies have shown that OSA increases overall mortality rates. OSA interrupts the normal pattern of sleep which causes tiredness and immediately increases the risk of having an accident while driving or operating machinery. Additionally, OSA (over time) places stress on the body created by low oxygen levels, and magnifies the risk of developing high blood pressure, heart attack, and stroke. Signs of OSA include daytime fatigue, morning headache, and not feeling rested even after an adequate time period of sleep. An overnight sleep study (polysomnogram) helps to distinguish between the two conditions. During a sleep study, measurements are taken of your heart rate and rhythm, blood oxygen levels, brain waves, muscle movements and breathing patterns.
Snoring and Obstructive Sleep Apnea are separate but sometimes associated disorders that result from upper airway obstruction. Snoring results from multiple factors that may include nasal airway obstruction, obesity, mouth breathing, enlargement of the adenoid, tonsils, and base of the tongue, and vibration of structures such as the uvula and soft palate. Obstructive Sleep Apnea (OSA), or cessation of breathing during sleep, may result from the same factors, but is a more serious health condition. Medical studies have shown that OSA increases overall mortality rates. OSA interrupts the normal pattern of sleep which causes tiredness and immediately increases the risk of having an accident while driving or operating machinery. Additionally, OSA (over time) places stress on the body created by low oxygen levels, and magnifies the risk of developing high blood pressure, heart attack, and stroke. Signs of OSA include daytime fatigue, morning headache, and not feeling rested even after an adequate time period of sleep. An overnight sleep study (polysomnogram) helps to distinguish between the two conditions. During a sleep study, measurements are taken of your heart rate and rhythm, blood oxygen levels, brain waves, muscle movements and breathing patterns.

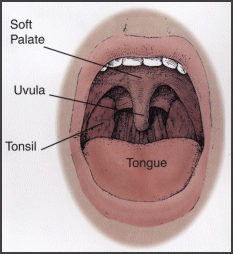 Surgery is considered for snoring when the effects of the noise become too intrusive. Surgical intervention for OSA is considered when weight loss has failed and the patient cannot tolerate or chooses not to wear CPAP.
Surgery is considered for snoring when the effects of the noise become too intrusive. Surgical intervention for OSA is considered when weight loss has failed and the patient cannot tolerate or chooses not to wear CPAP.